Fundamental Science
Spectroscopic OCT plus AI detects high-risk plaque in coronary arteries
Mar 24, 2026, 9:00 AM
出典: Physics World
<p>Artificial intelligence-based optical coherence tomography could improve long-term management of patients with coronary artery disease</p>
<p>The post <a href="https://physicsworld.com/a/spectroscopic-oct-plus-ai-detects-high-risk-plaque-in-coronary-arteries/">Spectroscopic OCT plus AI detects high-risk plaque in coronary arteries</a> appeared first on <a href="https://physicsworld.com">Physics World</a>.</p>
Details
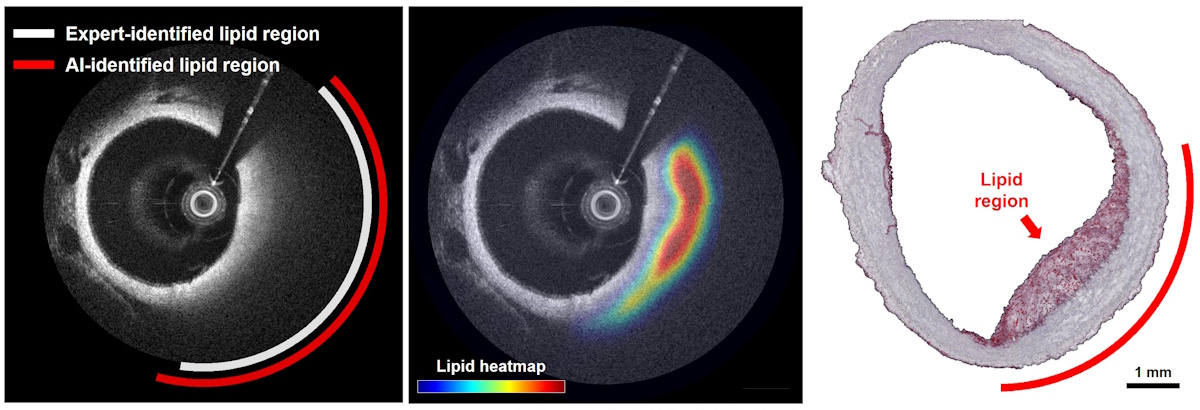
Identifying lipid-rich plaques inside coronary arteries is critical to assess a patient’s risk of having a heart attack. These fatty deposits adhere to the walls of blood vessels and, if they rupture, can trigger adverse cardiovascular events.
Currently, physicians use near-infrared spectroscopy and intravascular ultrasound (NIRS-IVUS) to quantitatively assess plaque lipid burden. Optical coherence tomography (OCT) is another intravascular imaging modality used during catheter-based procedures and provides micrometre-resolution visualization of plaque structure. But its diagnostic accuracy is limited by imaging artefacts and signals originating from non-lipid plaque components.
Researchers in Korea are developing a different approach: combining the biochemical specificity of spectroscopic OCT (S-OCT) with artificial intelligence (AI). This combination enables automated, composition-aware tissue characterization, and offers interpretable and annotation-efficient lipid mapping.
“By enabling efficient lipid screening and spatial interpretation, [the technique] establishes a scalable foundation for downstream assessment of lipid burden and clinically relevant plaque characterization, with potential utilization for automated risk stratification,” the researchers explain in Biomedical Optics Express.
Model training and validation
The AI-enhanced S-OCT system, which utilizes existing OCT systems without requiring hardware modification, incorporates an AI model developed by researchers at the Korea Advanced Institute of Science and Technology (KAIST) and the Multimodal Imaging and Theranostic Lab of the Korea University Guro Hospital. The AI model receives wavelength-dependent information from the OCT images and, by recognizing signal patterns associated with lipid-rich tissue, automatically highlights any suspicious regions in the image.
Team leader Hyeong Soo Nam from KAIST and collaborators created a dataset to train the AI model, using 848 lipid-positive and 622 non-lipid frames acquired from images of five rabbits with induced atherosclerotic plaques. They manually annotated each OCT frame to indicate lipid presence, and employed complex calibrated interferometric signals obtained through standard OCT processing to extract depth-resolved spectroscopic information for S-OCT. Finally, they applied a vessel region selection procedure with a depth range selected to focus the analysis on biologically relevant vessel regions with potential lipid content.
After training the deep-learning model, the researchers evaluated its performance in classifying lipid presence and spatial localization of lipid-associated regions, on both lipid-positive and non-lipid image frames. They also conducted histopathological validations to validate the predictions against ground truth, and compared the performance of the trained S-OCT model with an identically trained greyscale OCT-only model to assess the benefit of incorporating spectroscopic identification.
When assessing the relative importance of distinct spectral regions for lipid detection, the researchers discovered that training the model on a short-wavelength spectral subset (below 1300 nm) resulted in a higher lipid localization Dice score (a similarity metric) than a model trained on the long-wavelength band (above 1300 nm).
“This performance difference suggests the network relies more on spectroscopic features in the short-wavelength region, where lipid absorption shows a more pronounced spectral gradient,” they write. “The superior performance with short-wavelength data implies that the model effectively utilizes this spectral gradient, rather than relying on shared morphological features, to enhance lipid detection.”
The researchers validated their approach by imaging two rabbits with atherosclerotic plaques, and comparing the AI-generated predictions against histopathology results using lipid-specific tissue staining. The proposed model accurately localized lipid regions with strong spatial correspondence to histology, achieving a lipid localization Dice score of 83.9%.
“The results showed strong classification performance along with good spatial agreement with the pathological findings,” says Nam in a press statement. “By analysing wavelength-dependent information hidden in the OCT signal and combining it with AI, we were able to identify the presence and distribution of lipids within the vessel wall.”
“During a coronary intervention, this method could provide clinicians with additional information to support risk assessment, procedural planning and evaluation of treatment response,” Nam emphasizes. “Ultimately it has the potential to contribute to safer clinical decision making, more individualized treatment strategies and improved long-term management of patients with coronary artery disease.”
The team is currently working to improve the processing speed and robustness of their approach to make it more practical for real-time clinical use, and plan to perform validation studies using data from human coronary arteries. In addition, they aim to create a seamless method for integrating data reporting (the presence or absence of lipid plaque) into the clinical workflow.
The post Spectroscopic OCT plus AI detects high-risk plaque in coronary arteries appeared first on Physics World.
Related Knowledge
mentions
Optical Coherence Tomography (OCT)
Optical Coherence Tomography (OCT) is a non-invasive imaging technique that uses light waves to take cross-section pictures of the retina, allowing for detailed visualization of tissue structures. It is widely used in medical diagnostics, particularly in ophthalmology and cardiology, to detect abnormalities in tissues.
mentions
Machine Learning in Medical Imaging
Machine learning in medical imaging refers to the use of algorithms and statistical models to analyze and interpret medical images. This technology can enhance image quality, automate the detection of abnormalities, and assist radiologists in making accurate diagnoses.